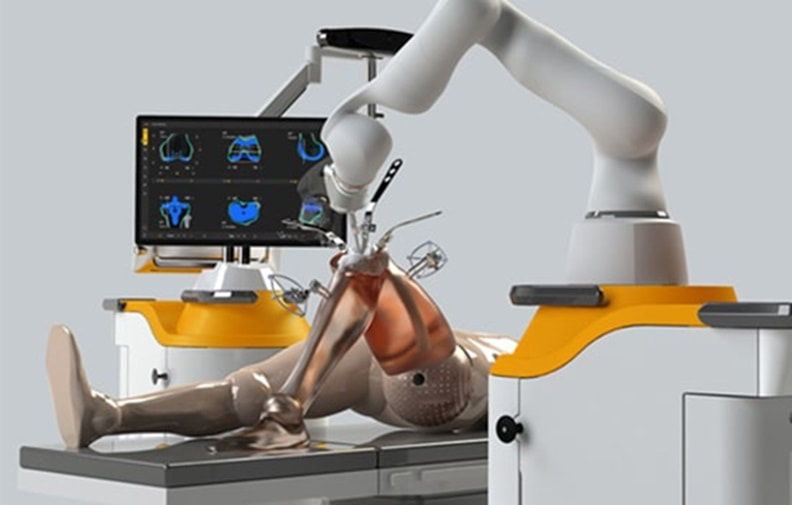
 Introduction Robotic knee replacement surgery has emerged as a groundbreaking advancement in the field of medical science. This innovative procedure combines the precision of robotics with the expertise of orthopedic surgeons to provide patients with improved outcomes and faster recovery times. In this article, we will explore the benefits of robotic knee replacement surgery and how it is revolutionizing the field of orthopedics. What is Robotic Knee Replacement Surgery? Robotic knee replacement surgery, also known as robotic-assisted knee surgery, is a minimally invasive procedure that utilizes advanced robotic technology to assist orthopedic surgeons during knee replacement surgeries. This procedure involves the use of a robotic arm, which is controlled by the surgeon, to perform the surgery with enhanced precision and accuracy. The Benefits of Robotic Knee Replacement Surgery 1. Enhanced Precision One of the key advantages of robotic knee replacement surgery is the enhanced precision it offers. The robotic arm used in this procedure allows for more accurate placement and alignment of the knee implant. This precision helps to optimize the function and stability of the knee joint, leading to improved outcomes for patients. 2. Customized Treatment Every patient is unique, and their knee replacement surgery should reflect that. Robotic knee replacement surgery enables surgeons to create a personalized treatment plan based on the patient's specific anatomy. By using advanced imaging technology, the surgeon can develop a 3D model of the patient's knee, which helps in determining the optimal size and placement of the implant. This customized approach ensures a better fit and alignment, leading to improved patient satisfaction. 3. Minimally Invasive Procedure Robotic knee replacement surgery is a minimally invasive procedure, meaning it requires smaller incisions compared to traditional open surgery. The smaller incisions result in less trauma to the surrounding tissues, reduced blood loss, and a faster recovery time for the patient. Additionally, the use of robotics allows for a more precise and targeted approach, minimizing the risk of damage to healthy tissues. 4. Faster Recovery Due to the minimally invasive nature of robotic knee replacement surgery, patients typically experience a faster recovery compared to traditional surgery. The smaller incisions result in less pain and scarring, allowing patients to regain mobility and return to their normal activities sooner. This accelerated recovery time is particularly beneficial for individuals who lead active lifestyles or have demanding physical jobs. Is Robotic Knee Replacement Surgery Right for You? Robotic knee replacement surgery is a highly advanced procedure that offers numerous benefits. However, it may not be suitable for everyone. Your orthopaedic surgeon in Delhi will evaluate your specific condition and determine if you are a good candidate for robotic-assisted knee surgery. Factors such as the severity of your knee condition, your overall health, and any previous surgeries will be taken into consideration. Conclusion Robotic knee replacement surgery in Delhi is a revolutionary advancement in the field of medical science. By combining the precision of robotics with the expertise of orthopedic surgeons, this procedure offers enhanced precision, customized treatment, and faster recovery times for patients. While not suitable for everyone, robotic knee replacement surgery provides a promising option for individuals seeking improved outcomes and a quicker return to their active lifestyles. Consult with your orthopaedic in Dwarka to determine if robotic-assisted knee surgery is right for you.
0 Comments
 Orthopedic specialists are medical professionals who specialize in diagnosing, treating, and preventing conditions related to the musculoskeletal system. This system includes bones, joints, muscles, ligaments, tendons, and other connective tissues. Orthopedic specialists play a vital role in helping individuals of all ages maintain and regain their mobility, reduce pain, and improve their overall quality of life. 1. Diagnosis Orthopedic doctors in Delhi are experts in identifying the root causes of musculoskeletal problems. They use a combination of physical examinations, medical history assessments, imaging techniques (like X-rays and MRIs), and sometimes laboratory tests to make accurate diagnoses. Whether it's a sports injury, chronic joint pain, or a complex condition, they have the knowledge and tools to pinpoint the issue. 2. Treatment Planning Once a diagnosis is made, orthopedic specialists develop personalized treatment plans tailored to each patient's unique needs. They consider factors like age, activity level, and overall health to determine the most effective approach. Treatment options may include physical therapy, medications, lifestyle modifications, or surgical interventions. 3. Non-Surgical Interventions Orthopedic specialists explore non-surgical treatments whenever possible. They may recommend physiotherapy in Dwarka to improve strength and flexibility, prescribe pain-relieving medications, or suggest the use of braces or splints to support injured areas. These approaches aim to alleviate pain and enhance function without the need for surgery. 4. Surgical Expertise In cases where conservative methods prove ineffective or when surgery is the best option, orthopedic surgeons in Delhi are skilled in a wide range of surgical procedures. This includes joint replacements, arthroscopy in Delhi, and complex reconstructive surgeries. They use advanced techniques and technologies to ensure the best possible outcomes for their patients. 5. Rehabilitation Recovery doesn't end in the operating room. Orthopedic specialists oversee the rehabilitation process, working closely with physiotherapist in Dwarka to help patients regain strength, mobility, and function. They provide guidance and support throughout the recovery journey, ensuring a smooth transition from treatment to everyday life. 6. Preventive Care Orthopedic in Delhi isn't just about treating existing conditions; they also emphasize preventive care. They offer advice on injury prevention, lifestyle modifications, and exercise routines to maintain musculoskeletal health. This proactive approach helps individuals reduce the risk of future orthopedic issues. 7. Pediatric Orthopedics Some orthopedic specialists specialize in pediatric orthopedics, addressing musculoskeletal conditions in children. They are trained to diagnose and treat conditions that affect a child's growth and development, such as scoliosis or congenital limb deformities. 8. Collaboration Orthopedic in Dwarka often collaborate with other healthcare professionals, including primary care physicians, physical therapists, and radiologists. This interdisciplinary approach ensures that patients receive comprehensive care that addresses both their orthopedic and overall health needs. In summary, orthopedic doctors in Delhi are indispensable in the field of medicine, playing a crucial role in diagnosing, treating, and preventing musculoskeletal conditions. Their expertise and dedication help individuals of all ages lead healthier, more active lives while minimizing pain and discomfort associated with orthopedic issues. If you're experiencing musculoskeletal problems, consulting with an orthopedic specialist can be a vital step toward improving your well-being and mobility.  Introduction: Pelvic floor fractures in males are relatively uncommon but can result from severe trauma to the pelvic region. The pelvic floor is a complex network of muscles, ligaments, and connective tissues that provide support to the pelvic organs, including the bladder, rectum, and prostate. Fractures in this area can lead to a range of symptoms, complications, and challenges. In this article, Dr Ashu Consul, Orthopaedic in Dwarka, explains the symptoms, problems, and treatment options for pelvic floor fractures in males. I. Causes and Risk Factors: Pelvic floor fractures typically occur due to high-impact accidents, such as motor vehicle collisions, falls from heights, or sports-related injuries. The most common risk factors include:
A. Acute Symptoms:
A. Chronic Pain: Some individuals may experience persistent pain in the pelvic area even after the fracture has healed. B. Urinary and Bowel Incontinence: In severe cases, damage to the pelvic floor muscles can result in involuntary leakage of urine or feces. C. Erectile Dysfunction: Nerve damage or disruption of blood flow to the penis can lead to difficulties in achieving or maintaining an erection. D. Infections: Fractures that penetrate the skin may create an open wound, increasing the risk of infection. IV. Diagnosis:
A. Conservative Treatment:
Physical therapy is essential for pelvic floor fracture recovery. Physiotherapist in Dwarka guides patient to focus on strengthening the pelvic floor muscles, improving mobility, and preventing complications like urinary incontinence or erectile dysfunction. Conclusion: Pelvic floor fractures in males can result from high-impact accidents and may cause a range of symptoms, complications, and challenges. Early diagnosis and appropriate treatment, including conservative management or surgery, can promote effective healing and reduce long-term problems. Rehabilitation plays a crucial role in restoring function and quality of life for those recovering from pelvic floor fractures. Understanding the symptoms, problems, and treatment options associated with these fractures is essential for both patients and the best orthopaedic in Dwarka to facilitate better outcomes. The hip is one of the joints most affected by injuries and degeneration of bones and cartilage. For this reason, adequate treatment carried out by an orthopaedic surgeon in Dwarka is important, to help avoid chronic injuries that affect the patient's quality of life.
What are the most frequent hip pathologies? The hip is the joint that serves as a union for the femur and the pelvis, it is one of the joints of the human body most affected by age. In many cases, hip pathologies are due to degeneration of the bones and tendons. Depending on the causes and symptoms, numerous hip injuries can be differentiated. One of the most common is hip bursitis, which is caused by inflammation of the synovial bag of the trochanter. The bursa protects the hip from impact and contributes to the mobility of the joint. Trochanteritis is characterized by inflammation of the trochanter, which is the protruding femur located in the upper part of the leg. In these cases, the patient often experiences radiating pain down the leg. Another of the most common hip injuries, especially among athletes, is hip groin pain. This pathology is produced by an affectation to the muscles of the inguinal area, caused by repetitive movements of the joint. Finally, hip osteoarthritis is one of the most common pathologies, which is characterized by the wear and degeneration of the hip bones, which can cause hip breaks or fractures. Causes of hip injuries Hip injuries do not have a specific cause, however, there are common causes observable in most patients with hip pathologies. First of all, muscular imbalances, that is, a progressive loss of strength in the hip muscles that increases the risk of injury. In these cases, it is common for the patient to also have a lack of flexibility in the area. In addition, as has been mentioned, one of the most frequent causes of hip pathologies is age , which accelerates the degeneration of bones and cartilage, increasing the chances of suffering a joint injury. Finally, overtraining or overexertion of the joint can be the cause of different injuries, since it causes muscle fatigue in the area. Symptoms of hip pathologies Usually, hip pathologies are manifested by acute pain in the joint that, on many occasions, radiates along the legs. It is common for this pain to appear accompanied by inflammation and immobility in the area, so the patient will experience difficulty in performing certain movements. Sometimes, the patient may have a sensation of heat in the area, especially in those cases in which inflammation appears. As well as weakness and immobility in the hip and legs. Diagnosis of hip injuries When the patient goes to the best orthopaedic in Dwarka manifesting symptoms of a hip injury, in the first place, he will undergo a physical examination, in which the possible existing inflammation will be studied, as well as those points in which there is greater pain. In most cases, especially those in which there is suspicion of hip rupture or fracture, it will be necessary for the patient to undergo diagnostic imaging tests, such as X-rays or magnetic resonance imaging, which will allow the available information to be expanded. Best treatments for hip injuries Once a complete diagnosis of the lesion has been made, the most appropriate treatment for each patient will be prescribed by orthopaedic in West Delhi. First of all, it is usually advisable to carry out a period of rest, which is accompanied by the application of cold in the area. The patient is usually prescribed an anti-inflammatory treatment, which helps to alleviate existing pain. In cases of inflammatory and muscular injuries of the hip, treatment with physiotherapy can offer good results, since it contributes to the strengthening of the area and, therefore, reduces the risk of future injuries. Surgery for hip injuries In cases of advanced osteoarthritis, or hip breaks and fractures, the most common treatment is surgery. There are different types of hip surgery, one of the most common is hip replacement in Delhi the implantation of a prosthesis made of synthetic material, which can assume the function of the joint. In other cases, it is decided to carry out a bone repair, through the implantation of screws and surgical material, which allows the joint to recover mobility. Tips to prevent hip injuries In those cases, in which hip injuries are caused by a degeneration of the joint, it is difficult to establish guidelines to avoid them. However, there are certain recommendations, which can be useful to protect the hip joint from injuries in the short and long term. First of all, it is important to control body weight, since the higher the BMI, the pressure on the joint will be greater and, therefore, the risk of degeneration of bones and tendons, too. In addition, it is important to treat the injuries correctly and applying a treatment prescribed by an orthopaedic doctor in Delhi. In this way, the relapse of injuries will be avoided, as well as the appearance of new pathologies. It is advisable to carry out exercises that help strengthen the hip musculature, as well as to avoid sports practices that suppose an excessive impact on the joint. As explained, the treatment of hip injuries is essential to avoid the chronification of pathologies. By following certain guidelines, the chances of developing the lesion can be significantly reduced. 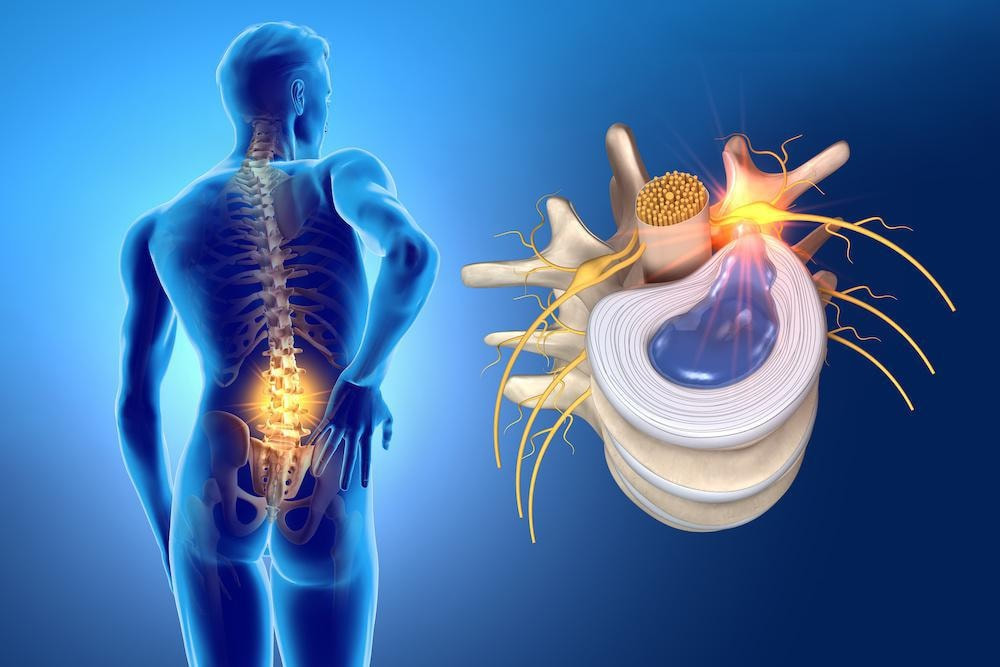 What is Disc herniation occurs when an intervertebral disc degenerates and deteriorates, causing the inner nucleus to leak into a weakened area on the outside of the disc. The weak point in the outer nucleus of the intervertebral disc is directly below the spinal nerve root, so a herniation in this area can put direct pressure on nearby nerves or the spinal cord. Therefore, herniated discs are sometimes a cause of radiculopathy, which encompasses any disease that affects the nerve roots of the spine. Dr Ashu Consul, best orthopaedic in Dwarka, consultant at Venkateshwara Hospital, adds that, initially, herniated discs can be confused with the following pathologies: “piriformis syndrome, facet arthropathies, deep gluteal syndrome, peripheral neuropathies, muscle trigger points and, in more severe cases, tumors”. Causes The vertebrae of the spine are separated by discs that cushion movement and leave space between the vertebrae. In the same way, they allow their movement, which makes it possible to bend down or stretch out. In addition, the vertebrae of the spine protect the spinal cord that comes from the brain and runs down the back to the lower back. The discs fulfill a very important function of cushioning and distribution of loads and any damage to them can be serious if not treated quickly. The disc can move out of place, that is, herniate, or rupture due to injury or stress. This can cause excess pressure on the spinal nerves resulting in pain, numbness or weakness in the patient. Normally, herniated discs are located in the lumbar region, with the second most affected area being the cervical discs (the neck). Symptoms A cervical disc herniation can cause pain in the neck, which in turn can radiate to the arm, shoulder, or can cause numbness or tingling in the arm or hand. Sometimes the pain can be dull, constant, and difficult to locate. In addition to this pain, the symptoms of herniated discs are the following:
According to Orthopaedic in Dwarka, “exercising regularly and appropriately is important. Also avoiding leading a sedentary lifestyle, being overweight and smoking helps prevent this type of back pathology. Finally, avoid unnecessary risks such as lifting heavy objects, improperly bending or twisting the lower back, or sitting or standing in the same position for many hours and in an unergonomic way. Types There are three degrees:
To diagnose a herniated disc, the orthopaedic doctor in Delhi will carry out a medical examination of the spine, arms and lower extremities. Depending on the region where the patient's symptoms are located, the orthopaedic in Delhi will look for possible numbness or loss of sensitivity. In addition, he will test your muscle reflexes, which may have been affected and slowed down or even disappeared. He will also study the patient's muscle strength and the shape of the curvature of the spine. On the other hand, the patient may also be asked to sit, stand or walk, bend forward, backward or sideways and move the neck, shoulders or hands. Diagnostic tests that can verify the existence of a herniated disc are:
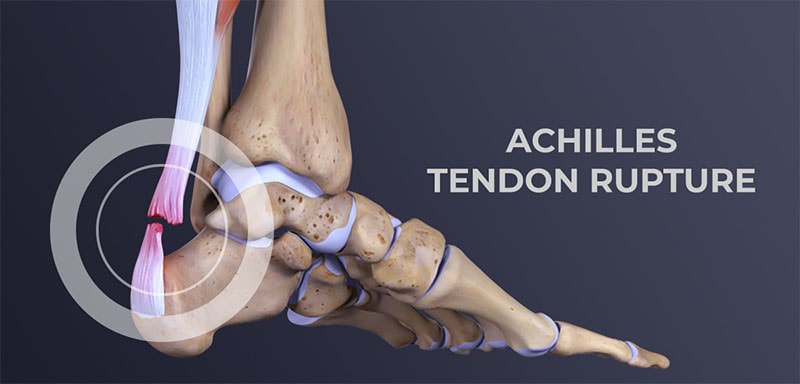
The first treatment given to patients with this condition is short rest and pain medication, followed by a period of physiotherapy session with physiotherapist in Dwarka. In most cases, almost immediate recovery occurs, but in other cases medication or injections may be required. In the case of corticosteroids, they are usually administered, above all, non-steroidal anti -inflammatory drugs to control pain and also muscle relaxants. Injections into the area of your back where the herniated disc is located can help control pain for a few months. In addition, these injections greatly reduce the swelling of the disc. The last option is microdiscectomy, considered as the surgery that is used to relieve pressure on the nerve root and allow the nerve to recover more effectively. This type of intervention does not entail great difficulty, since it is usually enough with a small incision and one night of admission. Regarding the therapeutic approach to herniated discs, Orthopaedic in West Delhi states that "one of the most important advances has occurred in the increased precision of diagnostic tools, which has made treatment much more effective and specific, both in management conservative as in the surgical. From the surgical point of view, the trend is towards minimally invasive, what we commonly know as microsurgery, so that the tissues suffer the least negative impact after the surgical intervention”. At what age do herniated discs usually appear? “Disc herniation can appear at any age, since its causes are multifactorial. Although, it begins to be more frequent in the range of 30 to 50 years of age. And they are more prevalent after the age of 50, where it is estimated that more than 80% of the population begins to show disc degeneration”, says orthopedic in Delhi. What is Achilles tendon rupture?
An Achilles tendon rupture or rupture occurs when the tendon “ruptures or tears” leading to separation or discontinuity in the tissues that make up the tendon. In terms of anatomy, the Achilles tendon, a sort of fibrous “ribbon” or “cord” that connects muscle to bone, is the largest and strongest tendon in the body that connects the calcaneus (heel bone) to the medial gastrocnemius muscles., lateral gastrocnemius and soleus muscles (popularly known as calf muscles or “leg belly” muscles). When the muscle contracts, it “pulls” the tendon, which in turn moves the foot. The rupture often reflects the previous existence of tendinosis phenomena caused by sports microtraumas or degeneration (aging) of the tendon. In most cases, the tear occurs at the bottom of the tendon (just above the heel), but it can occur anywhere along the tendon. In the presence of a healthy tendon, the lesion can appear in the bone or muscle. Total ruptures, partial ruptures We can generically classify Achilles tendon ruptures into:
See more information on treatments to better understand the different therapeutic approaches according to the extent of the lesion. Achilles tendon rupture - causes The Achilles tendon can lose elasticity and become “weak and thin” with age and lack of use. Then, it becomes prone to injury or breakage. Rupture is more common in people with pre-existing Achilles tendonitis (tendon inflammation). Repetitive tendinitis and the consequent calcifications are a risk factor for tendon rupture. Certain diseases (such as arthritis and diabetes) and medications (such as corticosteroids, for example) can also increase the risk of rupture. Rupture occurs most often in the middle-aged male athlete. The injury usually occurs during recreational sports that require impacts with the ground, running, jumping, etc. Most of the time, these are football, athletics, tennis, basketball, among others. Injury can happen in these situations as a result of traumatic dorsiflexion when the muscle is strongly contracted causing it to tear. Breaks can, however, also occur in everyday activities. For example, when falling from a significant height, when entering a pothole abruptly, traffic accidents, etc. Achilles tendon rupture - symptoms The signs and symptoms of Achilles tendon rupture are:
Achilles tendon rupture - diagnosis The diagnosis is made by the orthopaedic doctor in Delhi after collecting the clinical history, performing the physical examination and some complementary means of diagnosis (MCDT).Bottom of Form A simple test is to “stretch” the “calf or calf muscles” while lying on your stomach (Thompson test). In the impossibility of being able to elevate the foot, there is, most likely, a rupture in the tendon. This test isolates the connection between the “calf muscles” and the tendon and eliminates other tendons that may still allow poor movement. The orthopaedic doctor in Dwarka may order the following tests to confirm the diagnosis and to know in greater detail the location and degree of severity of the lesion:
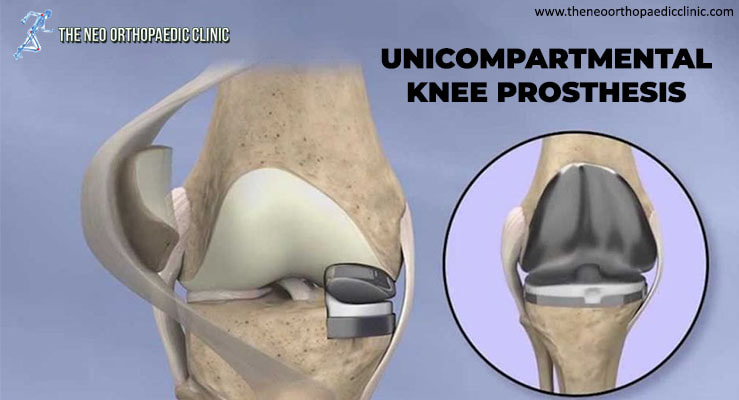
Achilles tendon rupture - treatment The objective of the treatment is to restore the function of the tendon, for this, it is necessary that the tissues that make up the tendon heal “united” with each other. In this way, it will be possible for the patient to return to the same level of activity before the injury. Regaining Achilles tendon function after an injury is critical to making walking possible. Treatment reflects a balance between tendon protection and initial movement. Protection is necessary to allow time for healing and to prevent further injury. Moving the foot and ankle is necessary to prevent stiffness and loss of muscle strength. We can divide treatment options into surgical and non-surgical. Conservative (non-surgical) treatment consists of a set of therapeutic attitudes aimed at healing the tendon and restoring its function without resorting to any type of surgical intervention. The choice between surgical and non-surgical treatment can be controversial in some cases. Both surgical and non-surgical treatment will require an initial period of approximately six weeks of immobilization. For most patients, both treatment options have good functional results. Non-surgical treatment Nonsurgical treatment is often used for non-athletes or for people with a low general level of physical activity who will not benefit from surgery. In the elderly and people with clinical complications, conservative (non-surgical) treatment should also be considered as a first option. Initially, a cast below the knee is performed with the foot in equinus (foot in marked plantar flexion, “down”). Although it is not routine, it is possible to perform an MRI to verify that the tops of the tendon are in contact. The cast is changed, at intervals of two to four weeks, to slowly stretch the tendon back to its normal length. This treatment usually takes 8 to 12 weeks. During this period, global strengthening and flexibility exercises are taught. Surgery (surgical treatment) Surgery on Achilles tendon rupture is often indicated in healthy and active people who want to resume activities such as walking, running, cycling, etc. Even those who are less active may be candidates for surgical repair of the tendon. The decision to operate should be discussed with your orthopaedic surgeon in Delhi. Surgery should not be performed if there is an active infection or damaged skin at or around the Achilles tendon rupture site. In addition, some diseases or lifestyle habits, such as diabetes, smoking habits, sedentary lifestyle, steroid use and inability to follow instructions after the operation, may be a contraindication for surgery. Surgical intervention for an Achilles tendon rupture is usually performed on an outpatient basis. This means that the patient is operated on and goes home the same day. We can identify two distinct surgical approaches: The first is to perform the intervention percutaneously, allowing to perform a minimally invasive surgery, through small incisions. A kind of needles with attached sutures are passed, allowing the Achilles tendon to be sutured. The second approach is the open approach (traditional method, where the surgeon makes an open incision to access the tendon). This starts with an incision made in the back of the leg, just above the calcaneus (heel bone). After the best orthopaedic in Dwarka finds the two ends of the torn tendon, these ends are sutured. The incision is subsequently closed. The surgical technique will be previously determined by the orthopaedic in West Delhi, depending on the type and location of the rupture, among other factors. In the postoperative period, regardless of the surgical technique chosen, the patient is immobilized with an equinus foot. Despite being a safe surgery, some complications can arise, such as risks associated with anesthesia, infection, damage to nerves and blood vessels and bleeding or blood clots, among others. A new rupture can also occur (recurrence). Recovery after surgery After the surgery, the patient is placed with a splint or a “plaster boot” from the foot to the knee. Usually, the patient cannot walk or put weight on the involved leg. Crutches, a walker or a wheelchair are used to allow the patient to remain mobile for the first few times. Patients are encouraged to keep the operated leg elevated above the level of the heart to decrease swelling (swelling) and pain. Patients are usually seen in the office two weeks after surgery. The splint or cast is removed, and the surgical incision is evaluated. Stitches are usually removed at this point if necessary. After two to six weeks, depending on postoperative protocol and orthopedic in Dwarka preference, patients may be allowed to begin performing some force. For this, a “hiking boot” can be used. Ankle movement is often allowed and encouraged. After six weeks, full-body strength is generally allowed. Physiotherapy in Dwarka will need to be started and is intended to restore ankle range of motion. Strengthening of the “calf muscles” and Achilles is gradually allowed as the tendon heals. It is usually possible to resume full activity after six months. Recovery time after surgery can extend up to a year, until the patient can achieve full rehabilitation. Even in cases where surgery is performed, the above-mentioned therapeutic attitudes are included in the rehabilitation plan. See more information on conservative treatment.  Hip arthrosis, also called coxarthrosis, belongs to a group of diseases called chronic degenerative diseases, that is, diseases that progressively evolve, affecting certain areas or tissues of the body. In the case of osteoarthritis of the hip, there is progressive wear and tear of the cartilage of the hip joint. This disease is also characterized by bone neoformation in the region where there was joint wear. These neoformed structures are popularly called parrot beaks. Risk Factors for Hip Osteoarthritis It is not known for sure why certain groups develop hip arthrosis, but it is known that some situations tend to increase the probability of developing this degenerative disease. Among these factors are previous diseases of the hip, such as epiphysiolysis, in addition to septic arthritis, congenital dislocation, femoroacetabular impingement, rheumatism, fracture sequelae, as a result of previous surgeries, etc. This pathology usually affects older people. In the case of previous diseases in the hip, it is called the pathology of secondary hip arthrosis. It is estimated that in the population over 65 years of age approximately 12% have symptomatic osteoarthrosis. Symptoms The main symptom of hip arthrosis is pain, located in the groin area. But the patient may report other symptoms such as difficulty performing simple movements such as bending down or bending, as well as joint stiffness and crepitus. Other symptoms are pain in the buttocks area and the pain may be present even after a period of rest, especially at night. Difficulty performing simple activities such as walking, climbing stairs, sitting or crossing the legs is present in cases of coxarthrosis. As coxarthrosis is a progressive disease, the signs and symptoms also have a progressive evolution, that is, they can start in a very mild and little limiting way, but progress to intense and very limiting. Thus, the first signs of coxarthrosis include joint stiffness, which starts bothering more in the morning, but tends to disappear during the day. In these cases, the limitation of movement is quite small. With the passage of time and the evolution of the disease, joint involvement also increases and, as a result, the stiffness becomes greater and tends not to disappear during the course of the day. Even the pain can even radiate to other places, such as the lumbar spine, for example. Rest no longer helps to improve the condition and the patient begins to feel pain in any location or position, feeling very uncomfortable even when lying down or standing still. The consequence of this is that the patient increasingly decreases the level of movement and when he moves, he limps, trying to transfer the load to the other side of the body that does not present the pathology. Although this seems like a temporary solution, it actually only worsens the situation, as it leads to muscle weakness in the leg and buttocks, which are extremely important musculature for hip protection. Thus, it is important that a professional is sought when the first symptoms appear, so that the diagnosis is established and a good treatment plan made, precisely to prevent the natural progression of the disease from occurring. Diagnosis of Osteoarthritis of the Hip The diagnosis of this pathology is the responsibility of the orthopaedic doctor in Dwarka. Unfortunately, many patients are slow to seek medical help, believing that the pain and the situation will spontaneously improve, which is not the case with a degenerative disease. Clinical evaluation is essential, with the professional collecting information about the pain history and medical history of that patient. In addition, some functional exams to check the patient's muscle capacity in the region are performed. It is important to check the muscle condition of the leg, buttocks and thigh, to establish the degree of evolution of the disease. Imaging tests may be ordered, such as X-rays and MRIs. These exams are important to be able to assess the degree of involvement of the joint surface. The exam of choice for diagnosing hip arthrosis is the AP radiograph of the pelvis, also called pelvic panoramic, and the lateral view of the affected joint. The other imaging tests are important when the orthopaedic doctor in Delhi wants to eliminate other possible causes of the problem. The reduction of the joint space, as well as the presence of bony prominences in the region, are factors that are investigated with the analysis of the image exams. Treatment of Hip Osteoarthritis For the treatment of coxarthrosis, it is important to point out that not all cases require surgery, and conservative treatment is an excellent alternative that should be considered because of its positive results. However, in some cases, depending on the level of joint involvement, surgery becomes unavoidable. Conservative treatment for hip osteoarthritis The approach should always be individualized and geared to the patient's lifestyle and expectations about treatment. Depending on the degree of pain presented by the patient, the orthopaedic in Dwarka may prescribe appropriate analgesics and anti-inflammatory drugs to reduce the acute pain. This is part of conservative treatment. Physiotherapy in the Conservative Treatment of Hip Arthrosis Physiotherapy in Dwarka is also indicated for pain reduction, since there are physiotherapeutic techniques that are quite suitable for acute pain. Among these physical therapy techniques, we can highlight electrothermophototherapeutic resources, such as laser, TENS and ultrasound. Other techniques include myofascial release and joint mobilizations. From the reduction of pain, it is possible to focus on a second moment of conservative treatment with the support of physiotherapy in Delhi, seeking muscle strengthening and range of motion. Activities such as water walking and water activities (hydrotherapy) can also be quite helpful. At first, the exercises should start without movement, only isometric contraction. Then, with light contraction, then with manual resistance, elastic resistance and finally, resistance with weights. Appropriate muscle strengthening for patients with coxarthrosis prevents the progression of the disease, as it makes the musculature absorb the necessary load from the patient's activities, preventing this load from being transferred to the compromised joint region. The result is an improvement in the patient's physical condition, with reduced pain and improved functional and movement capacity. Surgical Treatment for Osteoarthritis of the Hip In some cases, due to the degree of involvement of the hip joint, the surgical indication ends up being the best option for the patient with coxarthrosis. When there is a very large involvement of the joint region or in cases where conservative treatment has failed, the surgical option can be offered to the patient. It is worth remembering that every surgical process has risks and that the patient will still have to undergo a long physical therapy rehabilitation after the surgery. Therefore, orthopaedic in Delhi explains to the patient that, although the results of the surgery can be positive, physical therapy rehabilitation is essential. The most indicated surgery for cases of hip arthrosis is arthroplasty or hip replacement in Delhi, but the indication of the surgical procedure will depend on several factors, such as the patient's age, etiology, degree of activity and range of motion. In addition, it is important to check whether the disease is present in only one hip joint or in both. Surgical procedures can be divided into three types: - Osteotomies and arthroscopies: change the position of the hip bones; - Fusion of the hip joint, called arthrodesis; - Replacement of the hip joint with a prosthesis (arthroplasty). Obviously, the most invasive surgical procedure of the three described is the replacement of the hip joint with a prosthesis. There is no rule, but in general, less invasive procedures are recommended in early cases. Arthrodesis is now considered a disused technique. Arthroplasty, on the other hand, is considered one of the greatest successes in medicine in terms of surgery and there has been a lot of progress not only in the surgical technique but also in the materials to be placed as prostheses. Even so, arthroplasty is indicated for the most severe cases of joint destruction. During knee replacement surgery in Delhi, the damaged bone and cartilage are covered with metal and plastic components. In a unicompartmental knee replacement (also called a “partial” knee replacement), only part of the knee is covered. This procedure is an alternative to total knee replacement for patients whose disease is limited to just one area of the knee.
Because partial knee replacement is done through a smaller incision, patients generally spend less time in the hospital and return to normal activities sooner than patients undergoing total knee replacement. ADVANTAGES OF PARTIAL KNEE REPLACEMENT Several studies show that most patients who are suitable candidates for the procedure have good results with unicompartmental knee replacement in Delhi. The advantages of partial knee replacement over total knee replacement include:
DISADVANTAGES OF PARTIAL KNEE REPLACEMENT The disadvantages of partial knee replacement compared to total knee replacement include:
SURGERY CANDIDATES If your osteoarthritis has advanced and non-surgical treatment options are no longer relieving your symptoms, orthopaedic in Dwarka may recommend knee replacement surgery in West Delhi. In order to be a candidate for unicompartmental knee replacement, your arthritis must be limited to one compartment of your knee. In addition, if you have any of the following characteristics, you may not be eligible for the procedure:
YOUR SURGERY A partial knee replacement operation typically lasts between 1 and 2 hours. Partial knee replacement. There are three basic steps in the procedure:
COMPLICATIONS As with any surgical procedure, there are risks involved with a partial knee replacement. Your orthopaedic surgeon in West Delhi will discuss each of the risks with you and take specific steps to help prevent potential complications. Although rare, the most common risks include:
RECOVERY Hospital discharge. Patients with partial knee replacement generally experience less postoperative pain, less swelling, and have easier rehabilitation than patients undergoing total knee replacement. In most cases, patients go home 1 to 3 days after the operation. Some patients go home on the day of surgery. Weight support. You will begin putting weight on your knee immediately after surgery. You may need a walker, or crutches for the first few days or weeks until you feel comfortable enough to walk without assistance. Rehabilitation exercise. A physiotherapist in Dwarka will give you exercises to help maintain your range of motion and restore your strength. What is Patellar Instability or Patellar Dislocation?
The patella, formerly known as the kneecap, is the front bone of the knee, responsible for transmitting the strength of the thigh muscles. In some situations, this bone can move out of its normal location, called patellar instability or patellar dislocation, explains the orthopaedic in Delhi. If the patellar dislocation occurred for the first time, it is called a primal patellar dislocation. From the second episode, it is called recurrent patellar dislocation. What are the symptoms of patellar instability? When a patellar dislocation occurs, there is severe pain and an inability to mobilize the knee. It is possible to see and feel that the patella has moved out of place. Most of the time, the patella comes back into place on its own almost immediately. Rarely, a doctor needs to put it in place with a knee extension maneuver. After a patellar dislocation, there may be a feeling of insecurity with the knee, even without the patella clearly moving out of place. This sensation is called a patellar seizure. It is a very uncomfortable symptom, which can interfere with normal activities, says the orthopaedic in Dwarka. How and why does patella dislocation occur? Patellar dislocation can occur from trauma, such as a blow or twist to the knee, or without trauma, in a common movement of the joint. Some people have knee features that favor patellar dislocation. Among the main ones are:
The medial patellofemoral ligament is the structure that prevents dislocation of the patella. When the patella is displaced, it is injured or loosened. When the patellar dislocation is treated without surgery, what is expected is that this ligament will heal. In the surgical treatment of patellar dislocation, reconstruction of the medial patellofemoral ligament is performed in most cases, explains the orthopaedic surgeon in Delhi. Learn more about patellar dislocation treatments below. How is patellar instability diagnosed? The diagnosis of patellar instability is made through a careful assessment of the patient's clinical history and physical examination, complemented with imaging tests. The main test to be evaluated is magnetic resonance imaging, which shows indirect signs of dislocation, injury to the medial patellofemoral ligament, and the anatomical changes that favor instability. In addition, MRI is essential to look for cartilage lesions. Other tests, such as radiographs in special positions and computed tomography, are useful for evaluating the shape of the knee and predisposing factors, states the orthopaedic in west Delhi. How is patellar instability treated without surgery? In what situation is he indicated? In the case of a patient with an episode of patellar dislocation, both non-surgical and surgical treatment are possible. The decision for one or the other must be individualized, after a detailed discussion between the patient and the orthopaedic surgeon in Dwarka. Non-surgical treatment involves immobilization for a period, followed by rehabilitation focused on exercises to strengthen and control the thigh and hip muscles. The goal of successful non-surgical treatment is the absence of new episodes of dislocation and patellar apprehension, the feeling of discomfort or buckling caused by instability, explains the orthopaedic surgeon in Dwarka. In which cases is surgery indicated? Situations that indicate treatment with patellar dislocation surgery are:
What are patellar instability surgeries like? According to the orthopaedic surgeon in Delhi, there are several procedures available for patellar instability, which are chosen according to the characteristics of each patient, and there may be a combination of procedures. This concept of individualized treatment is known as à la carte treatment, influenced by the French school. These are the most common procedures performed for patellar dislocation.
Postoperative care depends on the technique used. They usually involve a period of support with crutches and a knee brace. However, from the beginning, it is already allowed to put the foot on the floor and remove the immobilizer to move the knee in most situations. Rehabilitation includes restoring knee mobility and restoring strength and control of the musculature of the thigh, hip, and trunk. Bursitis in the hip is an inflammation in a hip pouch, called a “bursa”. It is a relatively common problem and is known to cause pain and generate various discomforts for the patient. It is part of the great trochanter pain syndrome and is associated with hip tendinitis as well. Being treated by the best orthopaedic in Dwarka, this disease unfortunately leaves many patients with their movements reduced, as well as prevents the hip from being flexed, for example. It can be caused by several factors, bursitis is uncomfortable, but with the correct diagnosis can be easily treated.
Hip expert: knowing what bursitis is important to fight it!Bursitis is a problem that can appear in both sedentary people and sportsmen and happens because of repetitive movements and overloads in the hip joint. Knowing your symptoms, causes and treatment is essential to get rid of these limiting pains and avoid the causes of bursitis. With the correct follow-up with the orthopaedic in Dwarka, this nightmare can have your days numbered. Learn more about bursitis and stay tuned for symptoms. Pain This is the main symptom of bursitis and is present in almost all cases. The most common complaint of patients with this problem is pain in the lateral face of the hip. This pain worsens when sleeping on the inflamed hip. The sensation is burning pain and usually worsens if the patient does not change position. Discomfort for movement and pain to walk, get up and sit are also quite common, not to mention that staying for long periods of time in the same position can cause worsening of the pain as well. The pain of bursitis is characterized by radiating to the thighs, often confusing the patient, who thinks that the problem may be in another location. Limitation Slow movements, not being able to walk as before, having pain when tying shoes and cannot squat are the main signs of the limitation of bursitis. Because it is an inflammation of the bursas that are located on the lateral face of the joint, bursitis can actually cause problems in movements and in turn limit the daily activities of the patient. Swelling Bursitis can cause local swelling, which in turn can be felt manually by the patient. The location besides being palpable, may also be with increased temperature. Pain to the touch Touch pain also happens in bursitis. Often when touching the swollen region, the patient may feel pain. This happens because of the whole inflammatory process and also by the daily activities of the patient. Hip bursitis is usually very painful and limiting. The patient is usually very concerned about the symptoms, but as a correct treatment, the resolution prognosis is usually excellent. Causes of hip bursitisThe causes of the appearance of hip bursitis are varied:
How long does hip bursitis last?The duration of trochanteric bursitis cannot be determined in advance. In some cases, such as trauma, it can last for a short period of time, but sometimes if one is neglected it can become chronic. When the pain subsides, begin to move slowly back to normal movement. At this time, it is important to have the support of a physiotherapist in Dwarka who will indicate the exercises to be performed to improve movement in the area. With these simple actions, the bursitis will subside. But if it doesn’t, corticosteroid injections can be used, growth factors can be introduced to repair damaged tissues, or even combined with ozone therapy. The last option is surgery, if the previous methods are not effective. How to treat hip bursitis?In the treatment of hip bursitis, rest is essential, at least while the pain remains in its acute phase. Let your hip rest as long as possible. To do this, it may be convenient to use a cushion with an anatomical design and memory. This cushion distributes the weight, avoiding excessive pressure and achieving adequate pelvic stability. With it you will be able to rest the hip and relieve the pain. And when you sleep, it is best to do it on your back or on the opposite side of the affected area, placing some pillows between your knees. In addition, it is convenient to apply cold to the hip to reduce pain and inflammation. The orthopaedic in West Delhi will also recommend taking non-steroidal anti-inflammatory drugs. Without a doubt, the best treatment for hip bursitis is prevention. It is necessary to avoid that it appears for the first time or that new episodes arise. That’s why it’s important:
|
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. Archives
August 2022
Categories |

 RSS Feed
RSS Feed
